Connect with Thousands of Payers at an Affordable Price!
Flexibility and integrated EDI connectivity through our Medical Billing Software give your medical practice the right tool to eliminate lost claims, fast-track your submission, improve your payment velocity, improve reimbursement, and efficiently manage your denials.
SUPPORTED EDI STANDARDS
The most billing software allows you to integrate with only one EDI partner. At OmniMD, you can select from not only a variety of choices, but our flexible medical billing software allows selecting more than one at a time to address your business needs and goals.
You can choose from various clearinghouse options that offer both transactions and fixed plans.
INTEGRATED CLEARINGHOUSE BENEFITS
Insurance Eligibility
Our eligibility verification tool allows you to do on-the-spot (real-time) eligibility and benefits check at the point of service and enable batch eligibility for pre-visit verification.
Swift Speedy Clearinghouse Enrollment
You can get set up to use OmniMD RCM software and medical billing services within 3 business days of switching over to us for most commercial payers.
Direct User Support
Our partner portals offer all our customers direct assistance when they need it.
Claim Scrubbing and Electronic Remittance Advice
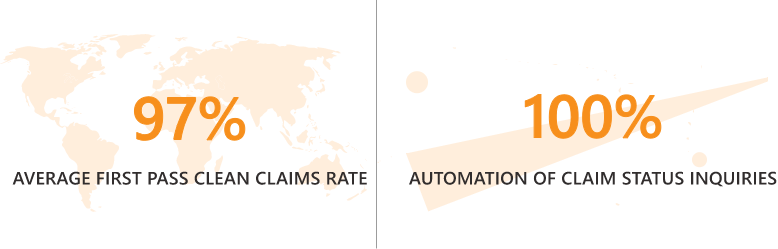
Every claim submitted through an integrated clearinghouse is checked for payer formatting, payer-specific guidelines, and coding edits to ensure compliance and coding accuracy. With an integrated clearinghouse, you get almost real-time embedded claim status to track your claims and avoid loss in transmission. Also, save time with automated processing of remittance advice.
Thousands of Payer Connections
Our integrated clearinghouse options offer all our customers thousands of payer connections and track of claims for all specialties—claim status and plan benefits at your fingertips.