It Sounds Too Good To Be True, But At Omnimd, We Simplify Every Step Of The Medical Billing Process And Ensure Every Claim Is Clean And Accurate. So That You Get Paid On Time And Every Time- Without Fail.
OMNIMD’S MEDICAL BILLING SERVICES

Yes, Medical Billing Services Can Be A Headache For Healthcare Practices. However, With Our Team Of Experts, You Can Rest Assured That Your outsourced medical billing services system Is In Good Hands. We Help You Recover Lost Revenue, End Claim Denials, And Get Paid Faster So You Can Focus On Delivering Quality Patient Care.
What’s More, We Are Always Up-To-Date With The Latest Outsourced Medical Billing Services Guidelines, To Be Confident That Your Claims Will Be Processed Without A Hitch. In Short, We Are Your One-Stop Solution For All Your Revenue Cycle Management Needs.
BILLING SOFTWARE COST CALCULATOR
Check out our Medical Billing Calculator and find where you may be losing valuable reimbursement dollars.
BENEFITS OF OMNIMD MEDICAL BILLING SERVICES
SYSTEM

Reduce Billing Errors And Denials
Eliminate denials and rejections.
Get paid faster and accurately

Improve Cashflow
Streamline revenue cycle management for faster payment and reimbursement

Enable Paperless Document Storage
Cloud-based storage and access to billing data and documents

Reduce Staff Size And Office Footprint
Minimize costs of staffing and office space with an outsourced team

Save On Billing Software Cost
We provide the software and integrate it with your technology systems

Transparent Process
Get a dashboard view of where we are in the revenue cycle process
BILLING & BANCHMARKING ANALYTICS
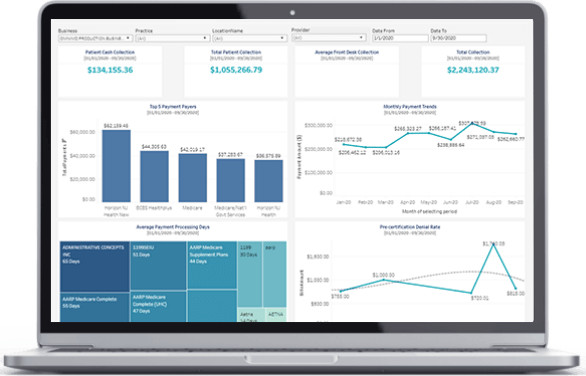
WHY CHOOSE OMNIMD
%
Healthcare Professionals
%
Healthcare Facilities
%
Customer Service Excellence
%
Patients Records
%
Uptime
%




